Bone is a living tissue that constantly renews itself. It is destroyed by cells called osteoclasts (bone resorption) and formed by cells called osteoblasts (bone formation).
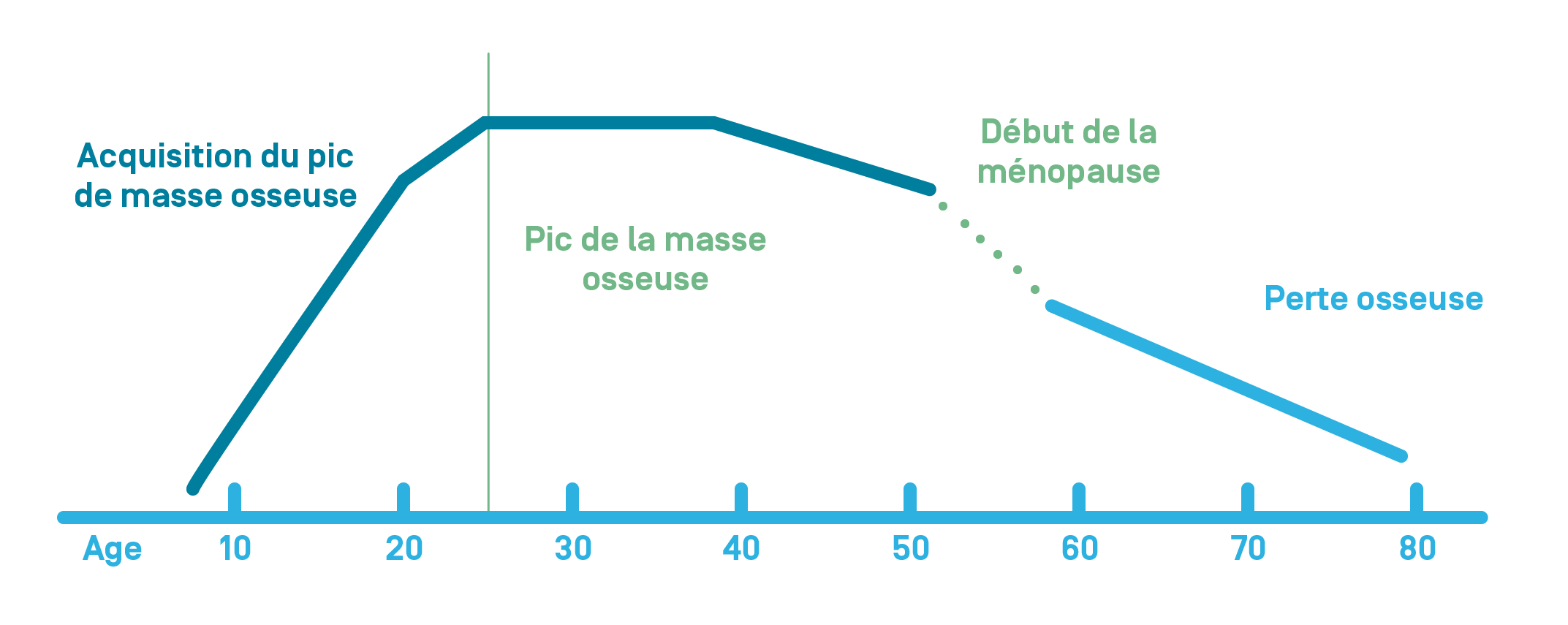
Once peak bone mass is attained (between age 20 and 30) the bone renews itself with a balance between bone resorption and bone formation. This is called bone remodeling.
With age, you see bone loss. This is accelerated in women during the menopause due to hormone deficiency.
Below a certain threshold of bone loss, this is called osteoporosis.
This bone loss is caused by an imbalance where resorption (bone destruction) predominates over bone formation.
Symptoms
Osteoporosis is a silent, painless disease. It is only when the person suffers a fracture that pain may be felt.
These fractures:
- can occur following a minor injury, for example due to falling over or a wrong movement,
- are more common in the vertebrae, hip, wrist, and shoulder,
- can lead to a loss of independence, a reduction in quality of life, and an increase in mortality.
Risk Factors
- Age: the older you are, the greater the risk of osteoporosis.
- Sex: women are at a greater risk of bone density loss due to hormone deficiency during the menopause. Osteoporosis does also occur in men however.
- Family history: if a close relative has fractured their hip in the past.
- Smoking and consuming an excessive amount of alcohol.
- Various medical conditions: digestive, rheumatoid, kidney, or endocrine conditions.
- Some medications, for example cortisone and certain treatments for breast or prostate cancer.
- Lack of movement.
- Being underweight.
- Falls are associated with an increased risk of fractures.
Diagnosis
Osteoporosis is diagnosed based on the results of a bone density scan, also known as DeXA (Dual-energy X-ray Absorptiometry). This measures bone density. This imaging technique uses very small quantities of X-rays, much lower than the amount used for spinal and hip X-rays.
Bone density (which is expressed in g/cm2) measures the calcium content of your skeleton. Your bone density is compared to the bone density of a healthy population without osteoporosis, with the difference expressed as a T-score.
The World Health Organization (WHO) defines osteoporosis as a T score ≤ -2.5.
The lower the T-score, the higher the risk of fracture. In other words, the less dense a bone is, the more fragile it is, which means it is at greater risk of a fracture.
The Examination Process
The examination will take place in the Nuclear Medicine department located on the lower ground floor of building B2 of Hôpital de La Tour. It will take about 45 minutes.
Once you have arrived at the secretarial office, a radiographer from the department will take charge of your care and explain the examination process. They will ask you to fill in a questionnaire that will help the nuclear medicine physician interpret your examination.
It will take 20–30 minutes to obtain the images (spine, hips, and/or wrist). Once we have ensured that they are of sufficient quality, you will be able to leave the department and resume your normal activities. The result will be sent directly to the referring physician and/or your primary doctor.
Reimbursement
In the following circumstances and when prescribed by your doctor, the examination is covered and reimbursed by your insurance:
- After a fracture caused by a minor injury (examination to detect bone fragility),
- When taking cortisone for several months or certain hormonal treatments,
- If your blood calcium level is too high (hypercalcemia) due to the glands (parathyroids) located in the neck not working properly (hyperparathyroidism),
- In the case of certain medical conditions that are responsible for poor absorption of calcium or a deficiency of ovarian hormones.
The Diagnostic Assessment Also Includes
- a medical consultation to assess your risk factors for osteoporosis,
- a blood test to detect potential causes of bone fragility.
Prevention
Some simple measures can prevent osteoporosis and fracture-related complications:
- Not smoking,
- Avoiding consuming excessive amounts of alcohol regularly (> two glasses of wine per day),
- Eating a healthy diet that is high in calcium and protein with sufficient amounts of vitamin D,
- Exercising regularly (for example walking, dance, or gym),
- Not being underweight,
- Preventing falls: for example, by making the necessary arrangements in your home, taking care of your eyesight, avoiding certain medications, and having physiotherapy.

Treatment
In addition to the preventative measures above, there are several medications that can effectively reduce the risk of fractures.
The referring physician will assess whether they are suitable for you depending on your individual fracture risk.
They will explain the most appropriate treatment for you and any potential side effects.
There are two different types of medication: medication to reduce bone loss, and medication that promotes bone building.
- Medication to reduce bone loss
Hormone replacement therapy
Estrogen receptor modulators
Bisphosphonates
Denosumab
- Bone-building medication
Teriparatide
Romosozumab
These medications are administered in tablet form, as an intravenous drip, or as an injection underneath the skin.
When Should You Contact the Doctor?
If you have osteoporosis risk factors (listed above).
If you have already suffered from a fracture.
If you have lost more than 3 cm in height or if you notice that your back is hunched, as this can be a sign of a vertebral fracture.
Care at Hôpital de La Tour
Hôpital de La Tour offers comprehensive multidisciplinary care for osteoporosis. Several medical specialties are involved in treating this disease, all of which are available on site.
In addition, Hôpital de La Tour is the only private clinic in Geneva that can offer a dedicated consultation for this condition.
Our state-of-the-art technology means we can perform the necessary imaging to diagnose the disease (DeXA) and fracture-related complications (X-rays, CT scans, MRI, bone scintigraphy, and SPECT-CT).
Treatment that require an injection or a drip can be administered on site.
The referring physicians for this condition are:
- • For a consultation: Dr. Isabelle Fabreguet
- • For a DeXA bone density scan (Nuclear Medicine department): Dr. med. Renaud Guignard.